Polycystic Ovarian Syndrome (PCOS), Infertility and Pregnancy
What is Polycystic Ovarian Syndrome?
- PCOS, short for polycystic ovarian syndrome, is a common cause of anovulation and female infertility
- It is also sometimes referred to as PCO (polycystic ovaries) or PCOD (polycystic ovarian disease).
Women with polycystic ovaries and fertility problems:
- Do not release an egg (ovulate) regularly
- Have ovaries that contain many small cystic structures, about 2-9 mm in diameter
How does normal ovulation work?
In a normal menstrual cycle with ovulation, a mature follicle – which is also a cystic structure – develops. The size of a mature follicle that is ready to ovulate is about 18 to 28mm in diameter.
- About 14 days after ovulation the woman would be expected to get a period if she is not pregnant
- The basic difference between polycystic and normal ovaries is that although the polycystic ovaries contain many small antral follicles with eggs in them, the follicles do not develop and mature properly – so there is no ovulation.
- Since women with polycystic ovaries do not ovulate regularly, they do not get regular menstrual periods
Symptoms of polycystic ovarian syndrome
A common scenario in women with polycystic ovaries is:
- Irregular menstrual cycles, called oligomenorrhea, and sometimes a total lack of periods, referred to by doctors as amenorrhea
- Onset of excess facial and body hair growth – hirsutism, in the teens or early 20s
- Gradually worsening of the excess hair growth over the years
Women with polycystic ovaries often have an excess amount of the male hormones testosterone and androstenedione – resulting in high testosterone levels in the blood. Women with PCO and high testosterone can have increased facial and body hair growth – called hirsutism.
Can I conceive with PCOS?
The good news is that the chance of getting pregnant with polycystic ovarian syndrome using fertility treatments is very good. The great majority of women with polycystic ovarian syndrome will be able to have a baby with fertility treatment.
For young women under age 35 with polycystic ovaries, the real question is more about which treatment will be effective – and not so much whether any treatment can ever work.
As far as the chances for pregnancy with PCOS – pregnancy statistics are difficult to give without knowing the details of the individual case.
Treatments for polycystic ovaries and infertility
Women with polycystic ovary syndrome usually need induction of ovulation to get pregnant.
- Information about options: PCOS Fertility Treatment Options and Success Rates
PCOS fertility treatment options include:
- Clomid for PCOS
- Femara (Letrozole) for PCOS
- Metformin for PCOS
- Injectable Gonadotropins for PCOS
- IVF – In Vitro Fertilization for PCOS
Diagnosing PCOS
How do doctors diagnose polycystic ovarian syndrome?
Diagnosing PCO with ultrasound – What does a polycystic ovary look like?
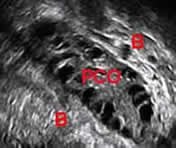
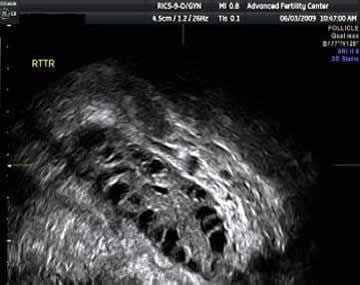
In a polycystic ovary, the numerous small cystic structures, also called antral follicles, give the ovaries a characteristic “polycystic” (many cysts) appearance on ultrasound.
Ultrasound Pictures: Normal Ovary vs. Polycystic Ovary
Ultrasound photo: Polycystic ovary with many antral follicles
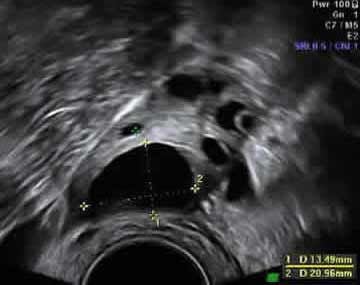
Ultrasound photo: Normal ovary with a single mature follicle
Yellow cursors measure the follicle. Fluid in the follicle is black on ultrasound.
Follicle wall contains a microscopic egg – ready for ovulation soon
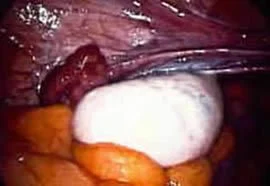
Surgery Photo: Enlarged polycystic ovary at laparoscopy
Surgery picture of a typical, enlarged polycystic ovary
The numerous small cysts are just under the thick outer capsule