Ovarian Hyperstimulation Syndrome, OHSS
Ovarian Hyperstimulation Syndrome (OHSS)
Ovarian hyperstimulation syndrome, or OHSS, is a condition that occurs when the ovaries become enlarged and fluid accumulates in the abdominal cavity. This condition typically appears a few days after egg retrieval or in early pregnancy.
Common OHSS Symptoms:
- Lower abdominal distention (bloating)
- Abdominal pain
- Nausea and possible vomiting
- Diarrhea
- Difficulty breathing due to pressure on the diaphragm from the ovaries and fluid buildup
Abdominal distention is common after ovarian stimulation, so it alone does not signify OHSS. The most effective approach to prevent OHSS is cautious administration of injectable medications.
How to Prevent OHSS with a Lupron Trigger
Significant OHSS occurs in a small percentage of women undergoing ovarian stimulation for IVF, especially those with polycystic ovarian syndrome (PCOS) or high antral follicle counts.
Mild OHSS is common and affects up to 35% of women undergoing ovarian stimulation. Mild and moderate cases are managed through observation, exams, and sometimes blood work, while severe cases may require hospitalization or paracentesis (removal of excess abdominal fluid).
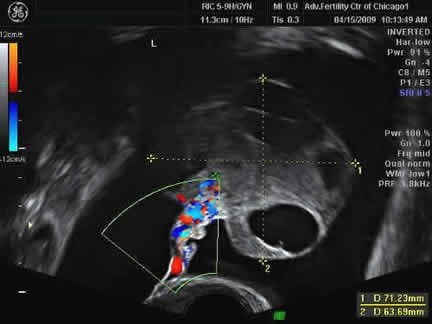
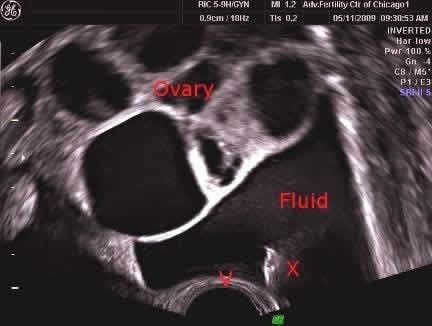
Ultrasound showing hyperstimulated ovary and free fluid in the abdomen
Why Does OHSS Occur?
OHSS is caused by increased vascular permeability, resulting in fluid leakage from blood vessels. High levels of vascular endothelial growth factor (VEGF) are believed to play a major role in triggering this process.
Management of OHSS
Mild to moderate OHSS is usually managed with patient education and pain medications. Severe cases may require a comprehensive evaluation, including:
- Physical examinations and ultrasounds to measure ovarian size and fluid levels
- Daily weight monitoring
- Blood tests for CBC, electrolytes, and creatinine
Hospitalization for OHSS
Severe OHSS may necessitate hospitalization under the following conditions:
- Severe abdominal pain
- Severe nausea and vomiting
- Very low blood pressure
- Severe blood test abnormalities
- Extremely low urine output
Paracentesis Procedure
Paracentesis is sometimes performed for moderate to severe OHSS cases to relieve symptoms by draining fluid from the abdomen. Ultrasound guidance is used to safely insert a needle and monitor the process.
Ultrasound-guided paracentesis for OHSS: Needle shown as white line next to the ovary
Preventing OHSS
OHSS prevention involves careful use of injectable FSH medications, especially for those at higher risk. Fertility specialists assess factors such as:
- High antral follicle count
- High AMH blood level
- High LH blood level or high LH to FSH ratio
Strategies for reducing OHSS risk include:
- Using a Lupron trigger to induce an LH surge instead of HCG
- Coasting for 1-3 days without FSH injections before the HCG trigger shot
- Lowering the HCG trigger dose to 5,000 units instead of the standard 10,000 units
Categories
About the AFCC Blog
Welcome to the Advanced Fertility Center of Chicago’s blog! Here, you will find information on the latest advancements in fertility care and treatments, including IVF, IUI, third-party reproduction, LGBTQ+ family building, preimplantation genetic testing, and more. Since 1997, we’ve used our experience and continuous investment in the latest fertility technology to help thousands of patients grow their families. Contact us today for more information or to schedule a new patient appointment.